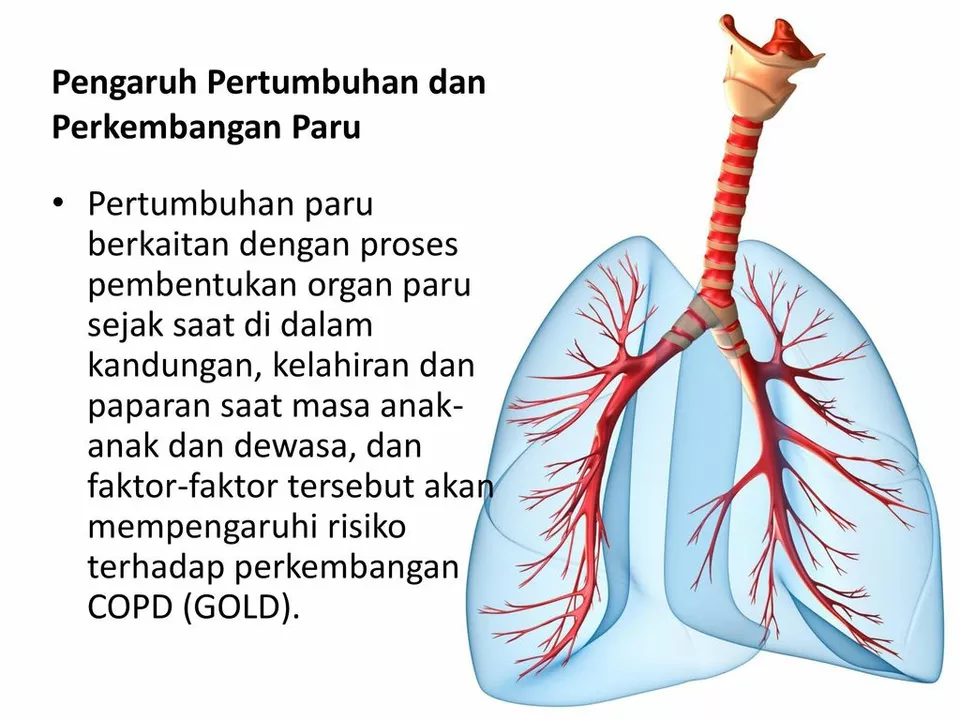
Chronic Obstructive Pulmonary Disease (COPD): What to know and what to do
Shortness of breath, a cough that won’t quit, or wheeze that shows up when you climb stairs — those can be COPD signs. COPD is a long-term lung condition that makes it harder to move air in and out. You can manage symptoms and slow progression with the right meds, habits, and support.
How COPD is diagnosed and treated
Your doctor will usually run a spirometry test (a simple breathing test) to confirm COPD and measure how bad it is. Treatment targets symptoms and flare-ups. Quick fixes are rescue inhalers like albuterol (Ventolin). Longer-term control comes from long-acting bronchodilators, inhaled steroids, and combination inhalers that reduce breathlessness and reduce flare-ups.
Some people do better on levalbuterol instead of racemic albuterol; check our Ventolin vs. Levalbuterol article for a clear comparison. If infections or resistant bacteria are a concern, there are antibiotic guides on the site that explain safer choices and side effects.
Daily habits that actually help
Quit smoking if you smoke — it’s the single best step to slow lung damage. Get your yearly flu shot and pneumonia vaccine when your doctor recommends them. Keep a small action plan for flare-ups: know your rescue inhaler, have a short course of oral steroids or antibiotics ready if your doctor prescribes them, and recognize warning signs like rapidly worsening breath, fever, or blue lips.
Pulmonary rehab is a game changer for many people. It’s supervised exercise, breathing training, and education that makes daily tasks easier and improves stamina. Even simple breathing techniques — pursed-lip breathing and controlled diaphragmatic breaths — cut anxiety during breathless moments.
Use inhalers correctly. Poor technique means less medicine where it’s needed. If you’re unsure, ask a nurse or pharmacist to watch you use your inhaler or spacer once — that quick check often makes a big difference.
Manage weight and stay active. Light cardio and strength work help your lungs and reduce fatigue. Start small: 10–15 minutes of walking or chair exercises, then add time as you feel stronger. If exercise makes you wheeze, our article on managing exercise-induced asthma offers warm-ups and alternatives that reduce symptoms.
Keep humidity and air quality in mind. Avoid smoke, strong fumes, and sudden temperature changes. A basic air purifier at home can reduce symptoms for some people. Also, track your breathing over time — note what triggers flares so you can avoid those situations.
If you have frequent flare-ups, talk to your provider about long-term oxygen therapy or advanced options. Make sure your medication list is reviewed regularly — some drugs interact or cause side effects that affect breathing.
Want more specific reads? Check related posts on inhaler comparisons, infection treatments, and practical COPD tips across the site. If you have questions about a medicine or a symptom, bring them to your next visit — a short conversation can change your daily comfort a lot.