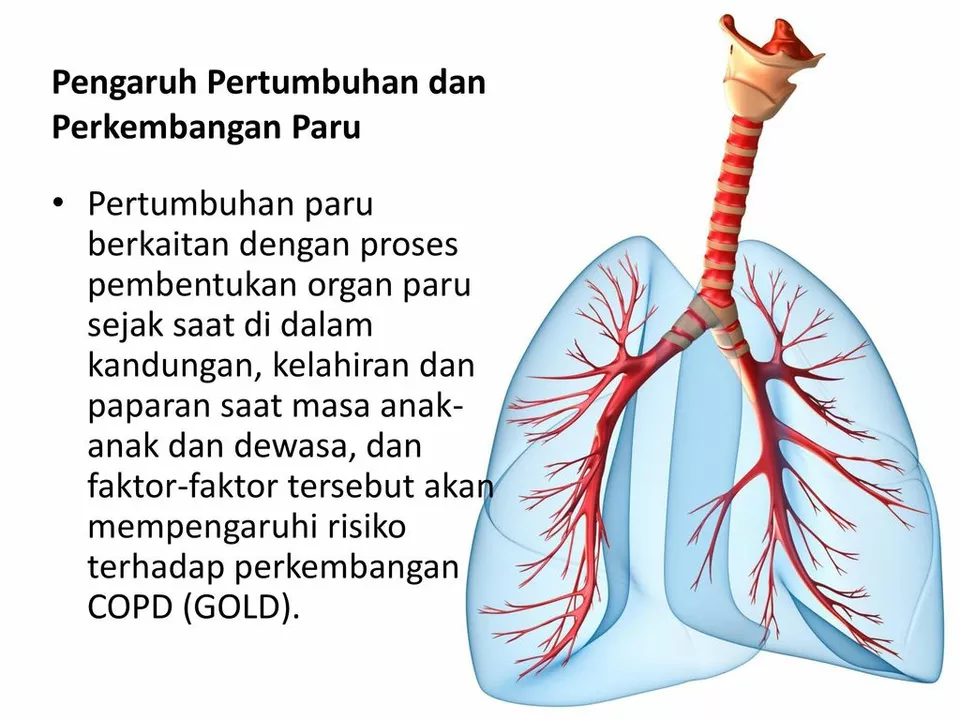
COPD Management: Practical Steps to Breathe Easier
If you or someone you care about has COPD, small daily changes make a big difference. The goal is clearer breathing, fewer emergency trips, and better days.
Start with your medicines. Take long-acting inhalers daily as prescribed and keep a short-acting rescue inhaler for sudden breathlessness. Learn proper inhaler technique—slow steady breaths with a spacer if needed—and ask your clinician to watch you use it once a visit. Refill prescriptions before they run out and track doses if you feel symptoms changing.
Build an action plan. Know what counts as a mild change, a worsening, and an emergency. Write down your usual medicines, symptoms to watch (increased cough, more sputum, trouble walking), and the exact steps to take at each level. Share this plan with family and your pharmacist.
Daily habits that help
Quit smoking and avoid secondhand smoke; stopping is the single best step to slow COPD. Get vaccines: annual flu and routine pneumococcal shots reduce serious lung infections. Stay active—pulmonary rehab or simple home exercises build strength and cut breathlessness. Aim for steady, low-impact activity like walking or cycling five times a week, starting slow and increasing as tolerated.
Practice breathing techniques such as pursed-lip breathing and diaphragmatic breaths to ease shortness during activity. Maintain good nutrition and hydrate well; losing muscle makes breathing harder, so prioritize protein and small frequent meals if eating becomes tiring.
Preventing and handling flare-ups
Know triggers: upper respiratory infections, air pollution, extreme cold, and allergens can spark flare-ups. Check local air quality and avoid heavy exertion when pollution is high. Use a pulse oximeter at home if advised, and call your doctor if oxygen levels drop or symptoms worsen despite rescue inhaler use.
If you catch a chest infection, start antibiotics or steroids only as directed. Many people have a rescue pack prescribed for early treatment—ask your clinician whether that’s right for you. Keep emergency numbers handy and arrange prompt transport plans for severe trouble breathing.
Work with your healthcare team. Regular spirometry, medication reviews, and check-ins help tailor treatment as your needs change. Discuss oxygen therapy, surgical options, or newer medications if symptoms progress. Ask about mental health supports; anxiety and breathlessness feed each other and simple counseling or breathing retraining helps.
When traveling, pack extra inhalers, a copy of your action plan, and a letter from your doctor if you use oxygen. Check airlines' rules for oxygen and bring sealed medications in original packaging. Learn how to clean your nebulizer or spacer and replace filters as instructed. Join a local COPD support group or an online community—shared tips and small wins keep motivation up. Keep a notebook of symptoms and questions for appointments every visit.
Small practical steps add up: keep inhalers nearby, plan daily walks, avoid smoke and bad air, stay current on vaccines, and carry a clear written action plan. These moves reduce hospital visits and improve confidence. If something feels different or worse, contact your clinic early rather than waiting.