Arrhythmia — What it feels like, when to act, and simple steps that help
An arrhythmia is any change in the heart's normal beat. Sometimes it feels like a flutter or skipped beat. Other times you might feel dizzy, short of breath, or suddenly very tired. Not every odd beat is dangerous, but knowing when to pay attention matters.
One common type is atrial fibrillation (AFib). AFib causes a fast, irregular pulse and raises stroke risk if untreated. Other types include premature beats (PVCs), supraventricular tachycardia (SVT), and slow rhythms that need a pacemaker. Each feels a bit different and needs a different approach.
How doctors check arrhythmias
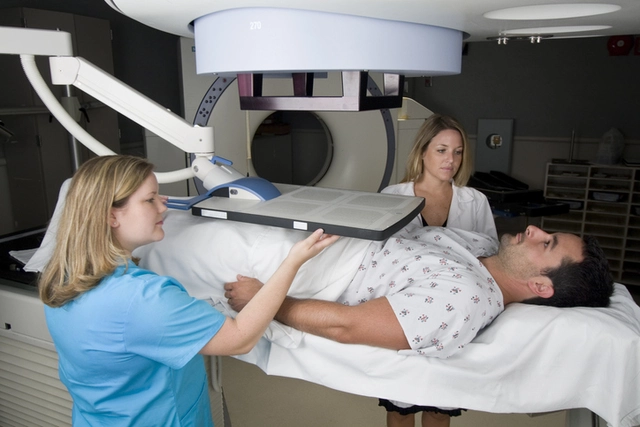
If you tell a doctor you feel palpitations, they'll usually start with an ECG. That’s a quick test that records heart rhythm. If the ECG is normal but symptoms continue, a doctor might order a Holter monitor (24–48 hours) or an event monitor you wear for weeks. An echocardiogram checks heart structure. Blood tests can catch thyroid problems or low electrolytes that trigger irregular beats.
Sometimes your doctor will recommend an exercise stress test or longer monitoring to catch rare episodes. Tests guide treatment. For example, AFib often needs blood thinners to prevent clots, while PVCs in an otherwise healthy heart may only need reassurance.
Simple steps you can take today
If you get a new, strong fluttering in your chest or faint, call emergency services. For milder palpitations, write down when they happen, how long they last, and what you were doing. This helps your clinician find triggers like caffeine, alcohol, lack of sleep, or stress.
Lifestyle changes can reduce episodes. Cut back on caffeine and energy drinks. Limit heavy alcohol. Stay hydrated and keep electrolytes normal if you sweat a lot. Practice slow breathing or short breaks when stressed. Regular sleep and moderate exercise often help too.
Treatments range from tiny to big. Medications like beta-blockers or approved antiarrhythmics control rate and rhythm. A cardioversion (a short controlled shock) can restore normal rhythm in some cases. For certain problems, catheter ablation destroys the small area causing faulty signals. Slow heart rates may need a pacemaker. Your doctor will explain risks and benefits for your situation.
Living with arrhythmia means regular checkups, taking meds as prescribed, and knowing emergency signs: chest pain, fainting, severe breathlessness. If you have AFib, talk about stroke prevention and whether blood thinners suit you.
Want to track symptoms? Use a simple notebook or a phone app to note episodes and triggers. That record often helps more than guessing. If you're worried, ask your doctor for monitoring—catching an arrhythmia on tape makes treatment faster and safer.
Questions about a specific medication or test? Bring the name to your appointment. Clear details make decisions easier for you and your doctor.