Prostate Cancer: What to Know Now
More than 1 in 8 men will get prostate cancer in their lifetime, yet most cases are caught early and are treatable. If you're worried or just want to be smart about screening, this page gives clear, practical info: what to watch for, how doctors check for it, main treatment choices, and simple lifestyle steps that can help lower your risk.
Screening and diagnosis
If you don’t have symptoms, screening usually starts with a PSA blood test and a digital rectal exam (DRE). PSA measures a protein made by the prostate; higher levels can mean cancer but also inflammation or benign growth. Talk to your doctor about when to begin—many men start at 50, but Black men and those with a close relative diagnosed young often start at 45.
When screening flags a concern, doctors often order a prostate MRI and then a biopsy to confirm cancer and measure aggressiveness (Gleason or Grade Group). Those tests help decide whether treatment is urgent or monitoring is safe.
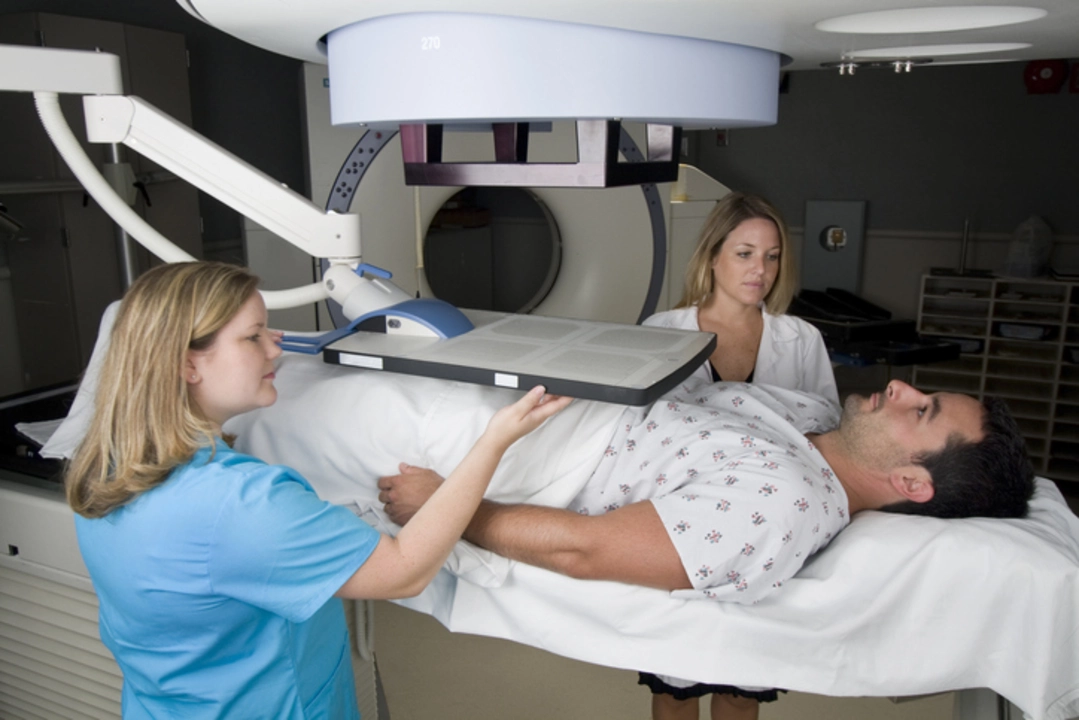
Treatment options and what to expect
Treatment depends on the cancer’s grade, stage, your age, and your health. If the tumor looks slow-growing, many men choose active surveillance: regular PSA tests, MRI scans, and occasional biopsies. This avoids side effects while keeping an eye on changes.
Surgery (radical prostatectomy) removes the prostate and can cure localized cancer. Radiation—external beam or brachytherapy—targets the tumor without removing the gland. Advanced disease may need hormone therapy (androgen deprivation) to lower testosterone, sometimes combined with chemo or newer targeted drugs. Each approach has trade-offs, so get a clear list of likely benefits and side effects from your doctor.
Side effects vary. The most common are urinary leakage, erectile dysfunction, and bowel changes after radiation. Hormone therapy can cause hot flashes, fatigue, and bone thinning. Rehabilitation and treatments exist for many side effects—pelvic floor exercises, erectile aids, bone-protecting meds—so ask about help early.
If you notice new urinary problems, blood in urine, sudden bone pain, or persistent pelvic discomfort, see a doctor. Also get checked if a routine PSA is rising over time. Early discussion gives you more options and better outcomes.
Simple steps that may lower risk: stay active, keep a healthy weight, eat more vegetables and healthy fats, and limit processed meats. These habits won’t guarantee prevention, but they improve overall health and can complement medical care.
Want specific guides, treatment comparisons, or practical tips for managing side effects? Browse our articles or contact a healthcare pro for personalized advice. Talking openly with your doctor about goals and risks will help you choose the path that fits your life best.