Living with cancer: practical tips to feel better every day
Living with cancer changes daily life fast. Treatments, tests, and side effects can overwhelm you, but small practical steps make a big difference. This page collects hands-on advice on symptom control, safety, mental health, and everyday planning so you can focus on what matters.
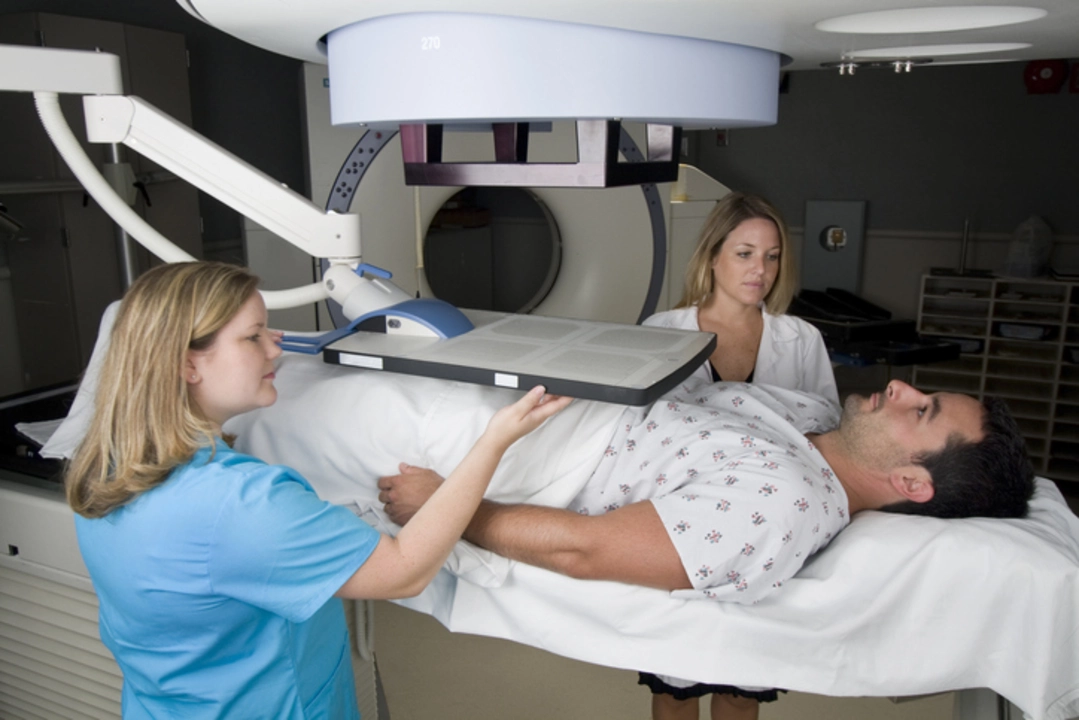
Managing physical symptoms
Pain, nausea, fatigue, and infections are common. For pain, bring a clear list of what helps and what makes pain worse to your care team; ask about options from nonsteroidal drugs to targeted prescriptions and physical therapy. For joint or arthritis-like pain, see our Celebrex guide to understand benefits and risks.
Nausea responds well to timing and small changes: eat small bland meals, avoid strong smells, try ginger or prescribed anti-nausea meds before treatment, and keep crackers by the bed. Fatigue improves with short walks, light strength moves, and planned rest—track your energy in a notebook to schedule the most important tasks when you feel best.
Infection risk is higher during some treatments. Wash hands often, avoid crowded sick settings, and update vaccines with your doctor’s ok. If you face bacterial infections, our articles on levofloxacin and clavulanic acid explain common antibiotic choices and why combinations sometimes matter.
Bone health and kidney-related calcium needs can change with treatment. Ask about bone-supporting options like alfacalcidol (Alfacip) if your doctor suspects risk to bones or vitamin D metabolism.
Coping, care and daily planning
Emotional strain is real. Share what you feel with a counselor, a support group, or a trusted friend. Small routines—regular sleep times, short walks, and hobby moments—give your day structure and calm. If medication for mood is an option, read our Wellbutrin and alternatives articles so your discussion with the clinician is informed.
Make a simple action plan: a phone list of team members, medication chart, symptom diary, and a power-of-attorney or emergency contact note. Keep all recent lab results and imaging dates in one folder so appointments stay efficient.
Ask about palliative care early. Palliative teams focus on symptom control and quality of life and can work alongside curative treatment. Also ask your care team about clinical trials if you want additional options; bring a list of questions to each visit.
Practical money and work advice matters. Check with social workers or patient navigators at your center for financial aid, disability paperwork, and employer letters. Simple adjustments at work—reduced hours, remote days, clearer deadlines—help when you’re low on energy.
Keep a medication list with doses, over-the-counter drugs, and supplements. Bring it to every visit so providers spot interactions — some cancer drugs mix poorly with common meds. Before starting any supplement or herbal remedy, ask your team; for example, some blood-thinning effects and herbal mixes change chemo side effects. A clear list prevents mistakes and saves time in emergencies.
For specific how-tos, read our guides on pain control, infection treatment, bone support, and mental health. Talk openly with your medical team and use reliable resources to make each day more manageable.